A prominent U.S. plastic surgeon says he believes breast implant illness affects a small but unpredictable subset of women, and that every surgeon should be discussing the illness with their patients.
Arizona plastic surgeon Dr. Richard J Brown took to social media Wednesday, May 11 to address a viral video by social media personality Bunnie Xo, whose implants grew mold after she had them explanted due to breast implant illness concerns.
Brown, social media’s most prominent plastic surgeon, shared with his 7.8 million followers that he’s explanted plenty of saline and silicone implants for breast implant illness patients but had yet to see mold growth in any of them.
“That being said, I believe in breast implant illness,” the board-certified surgeon told viewers.
“I have gotten a lot of slack from some of my colleagues because of that,” he says.
“I believe in breast implant illness. I have gotten a lot of slack from some of my colleagues because of that.”
Dr. Richard J. Brown, May 11, 2022
Surgeons are conflicted not only on whether breast implant illness exists as a diagnosable entity, but on how breast implants and the scar tissue capsules that form naturally around them should be removed from patients suffering from the often systemic illness they can cause.
This decades-long fray and evidence of financial conflicts of interest make their way into the public arena and have helped prompt suffering former patients to seek their own independent answers in droves.
As patient social media groups grow, so, too, do the number of surgeons and medical professionals (the most popular of whom do so anonymously) that publicly shame and attack them, reposting and ridiculing choice excerpts from the group’s founders and members, who now number more than 250,000 and have independently formed in more than 20 countries.
In some professional plastic surgery circles, publicly sharing one’s belief in the illness or gaining popularity as an excellent explant surgeon is grounds for ad hominem attacks, nevermind that no “plastic surgery journalist” will include the surgeon’s name and number in his or her carefully-culled rolodex.
Publicly tearing down a BII-believing surgeon’s intelligence, skill, motives and even looks are all on the table. “Bottom feeders” is how one surgeon, previously quoted by RealSelf and NewBeauty, publicly referred to these surgeons three weeks ago.
Brown believes the controversial illness affects a “very small subset of the population of women” and that it “doesn’t apply to the vast majority of women,” for whom he believes breast implants are safe.
Prompted by a potential patient’s question, the board-certified surgeon addressed the topic again days later.
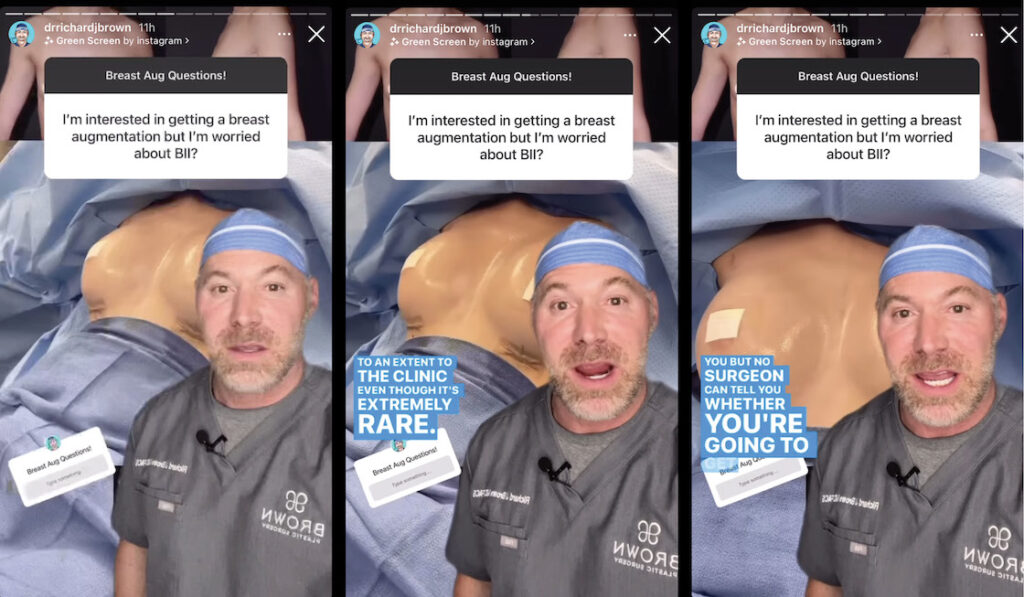
On Saturday, May 21, a viewer shared with the doctor that she was interested in breast augmentation surgery but was worried about breast implant illness.
“In this day and age,” the surgeon responded, “every surgeon should be discussing this to an extent in the clinic, even though it’s extremely rare.
“You need to be able to make the best informed decision for you,” he said, “But no surgeon can tell you whether you’re going to get it [BII] or not.”
In 2020, the latest year for which official statistics are available, 193,073 women had breast augmentation surgery in the U.S., according to annual data from the American Society of Plastic Surgeons.
“We all know what the benefits are with breast implants, they can provide a good aesthetic outcome, but the risks have been disregarded, downplayed or even hidden.”
Maria Gmitro, president and founder of Breast Implant Safety Alliance
That number, hefty as it is, also suggests that breast augmentation surgery may finally have fallen from its perch of popularity: For the first time in 15 years, it wasn’t the nation’s most popular plastic surgery procedure.
That year, 94,012 fewer breast augmentation surgeries were done.
While plastic surgery procedures across the board took a hit due to restrictions on elective surgeries, the number of breast augmentations performed reduced by twice the average drop per procedure attributed to COVID closures.
In contrast, of the 28 elective cosmetic surgery procedures that the ASPS tracks statistics for, breast implant removals (explant surgeries) saw the single greatest increase, reaching a 15-year high of 36,367.
Maria Gmitro, president and founder of the Breast Implant Safety Alliance (BISA), attributes the industry shift to the new ways in which information is reaching members of the public.
“Device manufacturers and plastic surgeons largely market to consumers,” she says, so while patients are aware of the benefits of breast implants, the risks “have been disregarded, downplayed or even hidden.”
The BISA founder cites a June 2019 report which revealed that between 1999 and 2019, breast implant makers had “concealed” more than 350,000 “apparent injuries” involving breast implants.
An FDA program that ended in June 2019 had allowed the adverse event reports to not reach members of the public.
In a typical year, 84% of women undergoing breast augmentation will receive silicone breast implants, and 16% will receive saline breast implants, all of which are enveloped in a silicone shell.
It’s the silicone that many female patients and a growing number of surgeons say is the probable cause of the constellation of symptoms some women experience after getting breast implants.
Among the most commonly reported symptoms of breast implant illness are: Fatigue, brain fog, joint and muscle pain, weakness, headaches, low libido, dry eyes, memory issues, anxiety, numbness and tingling in the extremities, hair loss, insomnia, heartburn, abdominal pain, weight loss, and an irregular heartbeat.
“The findings show that patients who self-report BII demonstrate a statistically significant improvement in their symptoms after explantation and that this improvement persists for at least 6 months.”
Breast implant illness study, 2022
A 2022 study involving patients with breast implants who were experiencing varying degrees of these symptoms before having their breast implants removed found a “statistically significant improvement” in their symptoms after explant surgery.
(Here again, argument persists as to the validity of the study’s other findings. But even while surgeons hold opposing views on the type of explant surgery required, parties on both sides agree that if a woman believes she is experiencing breast implant illness, breast implant removal is the solution.)
Breast implant removal surgery made RealSelf’s 2022 Most Worth It list as the seventh most worthwhile cosmetic procedure of the year, coming in three places ahead of breast augmentation surgery in 10th place.
“Individuals are feeling more comfortable with sharing their personal experiences,” Gmitro says of the uptick in breast implant illness and explant surgery coverage reaching the public, most of which comes from members of the public themselves. “Now patients can learn from each other and not only receive information from a plastic surgeon or device manufacturer that is trying to market to consumers.”
In February of this year, a Duke University research team called the trend a “paradigm shift,” and reported that from 2006 to 2019, Google searches for “breast implant removal” were up 235 percent, and for “explant,” up 527%.
“I applaud the plastic surgeons that are being more proactive about the issues of breast implant illness and BIA-ALCL,” Gmitro says, “but I will say that I wish it did not take so long because patients have been raising these issues for decades.”
